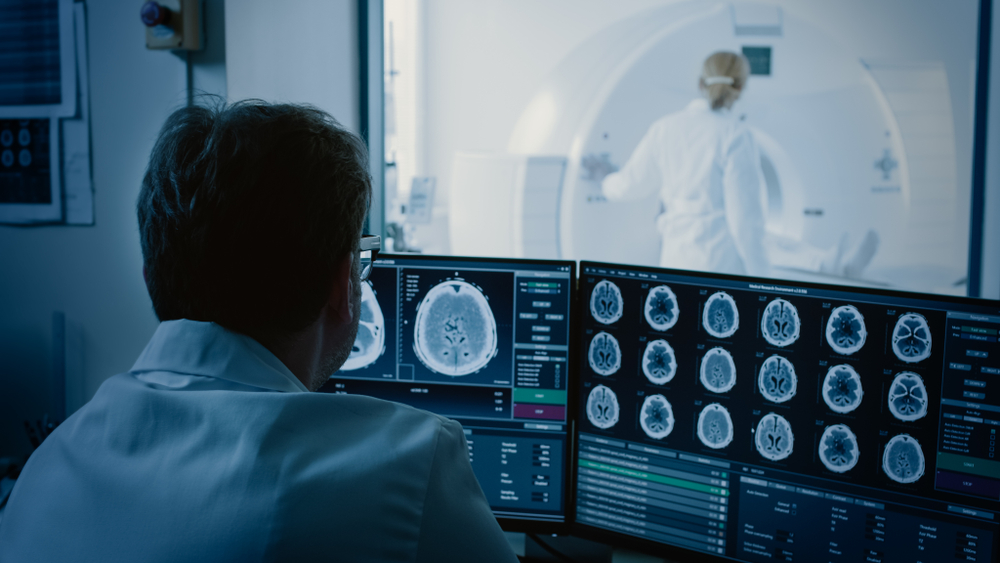
Diagnostic imaging plays a crucial role in modern medicine. But lurking behind every CAT scan, MRI, and X-ray lies a hidden scourge: unnecessary rescans. These repeated imaging procedures — caused by everything from technical glitches and inconclusive results due to sub-optimal patient positioning or operator technique or experience — not only drain valuable resources but also place undue stress on patients.
Thankfully, there are ways to address excessive rescans. It’s time to highlight this overlooked issue and work toward a more efficient, patient-centered approach to diagnostic imaging.
Scan and scan again
A rescan typically refers to the repetition of an imaging procedure — such as a CT MRI, ultrasound or X-ray — due to circumstances impeding the accurate interpretation of the initial scan. A rescan may be required for several reasons, including:
- Technical issues, from equipment malfunction to image artifact
- CD’s – still the most common method for exchanging studies – being unreadable by the recipient physician
- Inconclusive results yielded by the initial scan
These factors collectively contribute to an increasing prevalence of unnecessary rescanning each year. With each rescan comes significant costs and inconveniences for healthcare systems and patients alike.
Several studies and statistics reveal the magnitude of the problem of unnecessary rescanning. For instance, one peer-reviewed publication cites errors in “an estimated day-to-day rate of 3–5% of studies reported, and much higher rates reported in many targeted studies.”
Effectively, of the 1 billion radiologic examinations performed annually, 30-50 million are rescans. This figure — along with others probing the causes behind high rescan rates — underscores the substantial wastes associated with avoidable rescans.

The wastes and dangers of unnecessary rescans
Unnecessary rescans in diagnostic imaging have major implications, in terms of both the financial costs and waste of valuable healthcare resources. Each rescan incurs additional expenses, including equipment usage, staff time, and radiologist interpretations. These costs can add up quickly, burdening healthcare systems and diverting funds that could be allocated to other critical areas of patient care.
The cost also goes beyond the financial expense. One of the top risks associated with unnecessary rescans is the repeated exposure to radiation. Many imaging procedures, such as CT scans, involve the use of ionizing radiation. While the radiation dose from a single scan is typically considered safe, the cumulative effect of multiple scans can elevate the risk of potential radiation-related complications and adverse effects. Indeed, studies indicate that up to 2% of all cancers in the US are linked to CT scans.
Further, as the population ages, the demands on imaging equipment has driven up stress on the infrastructure and clinicians / technicians alike. Accordingly, burn-out rates among professionals is currently at alarming levels, leading to a severe shortage of radiologists. With the over 60 population set to grow nearly 50% by 2050 the current growth in radiology internship of 2.5% will likely deepen the problem.
Patient inconvenience must also be considered. Unnecessary rescans can impose increased stress, anxiety, and frustration due to prolonged waiting times for rescheduled scans, additional visits to the imaging center, and potential delays in receiving a diagnosis. Moreover, excessive rescans can lead to longer wait times for patients who require initial scans delaying their diagnoses and treatment plans.
Strategies for reducing rescans
While the medical field has largely accepted rescans as “part of the process,” modern innovations have unlocked opportunities to mitigate the need for rescans by resolving pain points before, during, and after the initial scans. Here’s how:
- Embrace advancements in imaging technology. For example, TeleRay enables remote specialist consultation during initial scans, decreasing errors caused by operator inexperience or technical glitches. Additionally, the integration of machine learning (ML) and artificial intelligence (AI) algorithms improve speed and accuracy of diagnosis.
- Implement standardized protocols. By adhering to well-defined and widely accepted protocols, such as positioning guidelines, imaging parameters, and acquisition techniques, providers can ensure consistency and optimize scan quality. Standardization minimizes variations in imaging practices and facilitates better comparability between studies.
- Foster interdisciplinary collaboration. Encouraging an open dialogue and providing clear communication channels allow for a better understanding of clinical indications and patient history, reducing the likelihood of misinterpretation or incomplete information. Radiologists can offer guidance to technicians during scans, ensuring optimal image acquisition, while referring physicians can provide comprehensive clinical information to enhance the accuracy of interpretations.
- Offer continuous education and training. Radiologists, technicians, and other staff members should be well versed in the latest imaging techniques, quality assurance measures, and protocols. Continuous education and training can decrease technical errors and increase the efficiency of initial imaging.
Mitigate the scourge of rescans
Unnecessary rescans pose a considerable burden on healthcare systems, patients, and resources. By embracing advancements in imaging technology, implementing standardized protocols, and fostering interdisciplinary collaboration, providers can take steps toward reducing rescans. While every scan won’t be viable, in the modern era, there’s more opportunity than ever to get it right the first time.
Learn how TeleRay can help healthcare providers manage medical imaging more efficiently. Book a demo today at teleray.com.